
Wellington Eye Centre Optometrist
Spring is the season of hope, budding flowers, bouncy lambs and the end of winter! But for those who suffer from hay fever, it can be a real drag.
You may have already started to experience itchy eyes and runny noses as the worst of winter is hopefully behind us. With the change of season just around the corner, now is the perfect time to learn about allergies and how they affect your eyes.
What is an allergy?
Allergy is one of the ways a body’s immune system reacts to certain substances. This reaction is exaggerated and causes damage to the tissues of the body.
A substance that triggers an allergic response is called an allergen. These allergens could be food, pollen, insects, ticks, fur, dust or even some medications. Certain people can become hypersensitive to some of these substances, while the same substance can be harmless to others.
How do allergies affect eyes?
Allergies can often cause a lot of discomfort for eyes. When the lining of the outer eye and eyelids reacts to an allergen, you can experience the following symptoms:
- Watery eyes
- Discharge from the eyes
- Puffy eyelids
- Dark circles under the eyes
- Itchy eyes
- Burning eyes
- Red eyes
- Light sensitivity
- Blurred vision
- Contact lens discomfort
What is hay fever?
Hay fever (or allergic rhinitis) is the name given to allergic reactions caused by airborne allergens, such as pollen. When an allergen like pollen comes into contact with the outer surfaces of the eyes, the conjunctiva, the cornea or the eyelids, it might inappropriately stimulate the immune system. The immune system is designed to protect the body from infections like viruses and bacteria, but it can get confused and can misidentify an allergen (such as pollen) as a harmful substance.
Hay fever is common and the symptoms are similar to those of a cold. They could be:
- Sneezing
- Blocked nose
- Runny nose
- Itchy nose
- Watery eyes
- Itchy eyes
- Itchy roof of the mouth
- Sinus pressure

How to manage eye discomfort
One of the best ways to reduce your allergy or hay fever related symptoms is to reduce your exposure to the pollen or allergen.
1. Drive with windows up, especially on windy days.
This reduces the amount of pollen that you encounter.
2.Close windows at home.
Especially on windy days, or in the morning from 5-10 am as this is when pollen is most likely to be in the air.
3. Avoid wearing contact lenses
Contact lenses physically rub against the surfaces of the eye, the cornea, the conjunctiva and the eyelids. Mechanical irritation like this can make an inflamed eye worse and can contribute to the release of histamine from the cells active in the immune response. Contact lenses can also trap allergens between the eye and the contact lens, increasing their contact time and increasing the chance of an allergic reaction.
4. Take antihistamines
Oral antihistamines, prescribed by your GP or over the counter from your Pharmacist can reduce your symptoms, but they do have side effects, so make sure you chat to a trained professional before taking them.
You can also get antihistamine eye drops, which are very helpful in controlling these symptoms. Ask your GP, Therapeutically endorsed Optometrist or your eye specialist to prescribe you antihistamine eye drops.
5. Use clean pillowcases
Replacing your pillowcases and facecloths regularly helps get rid of any dust or pollen that might have built up on the surfaces or in the weave of the fabric. This is even more important if you have pets that might share the bed!
6. Air conditioning
Air conditioners can transfer airborne pollen into the circulation of your home, office or car. Either turn the air conditioning off, or alter the settings so they are only re-circulating air already in the space, not getting fresh air from outside.
7. Avoid rubbing your eyes
Rubbing your eyes, or itching your skin releases histamine from the cells. The histamine then triggers the allergic response even further. A cold facecloth held gently over your closed eyes can help suppress the urge to rub your eyes. Antihistamine medications may also help.
8. Wash hands frequently
Washing your hands helps reduce the amount of allergens on your hands, whether that be pollen, dust or animal fur. Really important, especially if you are itching your face or rubbing your eyes!
9. Wear Sunglasses when outside
Sunglasses, safety glasses or even goggles will act as a barrier between your eyes and the pollen in the air. They help reduce your exposure to the allergen and can help reduce your body’s response.

Eyedrops for Hay fever and allergy sufferers.
Most anti-allergy eye drops are available over the counter from pharmacies, but not from supermarkets.
Patanol (Olopatadine) is the anti-allergy drop most frequently recommended for all levels of allergic eye conditions. Patanol is only available on prescription, it is an antihistamine and a mast cell stabiliser. If you have run out, you might be able to get a repeat prescription from your GP or Optometrist, or you could try the over the counter option of Zaditen, which has a similar effect.
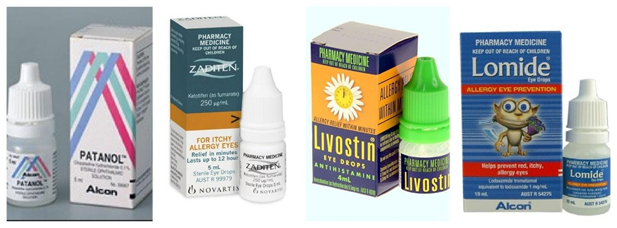
There are some allergy drops available over the counter, so no prescription is required. For most hay fever sufferers the antihistamine eye drops Zaditen or Livostin can be effective. There is also Lomide, a mast cell stabiliser eye drop, that is also available over the counter.
Not all anti-allergy eye drops are antihistamines or mast cell stabilisers. There is a group of eye drops that act in a very different way, called vasoconstrictors or decongestants. Albalon (and Albalon-A), Clear Eyes (and Clear Eyes-A) and Naphcon (and Naphcon-A) will usually help reduce redness, itchiness and swelling but they aren’t recommended for people with some forms of glaucoma, or with risks factors for angle-closure glaucoma. They also aren’t recommended for long term use, so if you’ve not used them before check-in with your eye care professional.
Can you get laser eye surgery if you suffer from allergies?
You may not even know you have hay fever and allergies. Have you ever had that early morning irritated nose, stingy eyes or just feel a bit off, like you had a cold brewing but it never manages to eventuate? That could be hay fever.
Even the mildest hay fever could mean your eyes are slightly inflamed. If you irritate an eye that is already slightly inflamed, the reaction can be far greater than you expect. Since laser vision correction is physically going to irritate the eyes, it pays to treat any other causes of inflammation before you have surgery. So eyes with even a little bit of allergy or dry eye related inflammation warrant a close check and at times, treatment.
Here at the Wellington Eye Centre, we assess your eyes closely before you undergo any form of eye surgery. One of the things we are looking for is the level of inflammation present on the outer surfaces of your eyes. Inflammation can be caused by numerous things; infection, auto-immune conditions, contact lens wear, allergy, hay fever, eczema, dry eye or injury.
Conditions like hay fever, asthma or eczema are also known collectively as atopy. People with atopy have a higher chance of developing an eye condition called Keratoconus. If you do have keratoconus, you will not be able to have laser vision correction. But you may be suitable for corneal cross-linking.
Can you keep taking allergy medications before surgery?
This depends on the type of medication. Antihistamine tablets can generally be taken until your eye surgery. However, you will be required to stop using eye drops 48 hours before your surgery. If you are taking any eye drops, let your laser surgeon know.
If you are using any creams for your eczema, be aware that you should only use steroidal creams very sparingly, especially around the eyes. Before surgery, and for one week afterwards, you should avoid putting any creams, medicated or otherwise, near your eyes.
How can your Optometrist help?
If you’re thinking of having laser vision correction surgery, but think you have eyes affected by allergy or hay fever, your Optometrist can help by assessing your eyes for levels of inflammation. Most Optometrists can then help reduce those levels with advice on contact lens wear and care, prescribing eye drops (antihistamine, anti-inflammatory or lubricating eye drops) or referring you to an Eye Specialist, such as Dr Andrew Logan.
Once you have had your free assessment for laser suitability, the next appointment is the medical assessment. At that appointment, our Optometrist or Ophthalmologist can advise you on your level of inflammation and the best ways to combat that. Although it is beneficial to turn up to that appointment with any inflammation already under control.
Any questions?
If you have any questions about your allergy or hay fever and how it might influence your chances for laser vision correction, please get in touch via email or phone 0800 733 327!

Vitamins For Good Eye Health and Vision

Blue Light, Evil or Essential?

Age Related Macular Degeneration (ARMD)

Everything You Need To Know About Dry Eye
Low-Level Light Therapy for Dry Eyes
Why we recommend Dry Eye Treatments before your Laser Vision Correction

Vitamins For Good Eye Health and Vision

How Much Does Laser Eye Surgery Cost in 2026?

Blue Light, Evil or Essential?

